J.ophthalmol.(Ukraine).2021;4:86-87.
|
http://doi.org/10.31288/oftalmolzh202148697 Received: 11 January 2021; Published on-line: 16 August 2021 Lens subluxation in a patient with homocystinuria. Case report Garduño-Vieyra Leopoldo, Flores Escobar Bruno Clínica Ophthalmology Garduño; Irapuato, Guanajuato (Mexico) E-mail: brnfelm9@gmail.com TO CITE THIS ARTICLE: Garduño-Vieyra Leopoldo, Flores Escobar Bruno. Lens subluxation in a patient with homocystinuria. Case report. J.ophthalmol.(Ukraine). 2021;4:86-7. http://doi.org/10.31288/oftalmolzh202148697 Homocystinuria is an inborn error of metabolism caused by cystathionine b-synthetase deficiency, with autosomal recessive inheritance. The clinical picture is characterized by skeletal changes, mental deficit, lens subluxation, and a tendency to thromboembolic phenomena. The case of a 35-year-old male patient with a marfanoid habit, eviscerated right eye, and abrupt loss of visual acuity of the left eye is reported, showing lens luxation; the determination of plasma homocysteine was reported elevated 285μmol / L (5-16μmol / L), confirming the diagnosis of homocystinuria. The management is multidisciplinary, the ophthalmological treatment required vitrectomy. Кey words: homocystinuria, lens subluxation, Marfan syndrome, vitrectomy
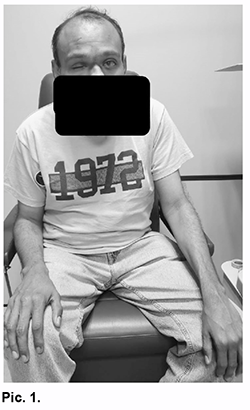
Introduction Homocystinuria is an innate error of metabolism caused by a deficiency of the enzyme cystathionine b-synthetase (autosomal recessive), characterized by the accumulation of homocysteine and methionine in the blood, in addition to increased excretion of homocysteine in the urine; It mainly affects the central nervous, vascular, skeletal and ocular systems, with an incidence of 1: 300,000 to 1:60,000 in our country [1, 2]. The clinical picture is characterized by skeletal changes, mental deficit, lens subluxation, and a tendency to thromboembolic phenomena. The management of lens subluxation should be performed by an ophthalmologist, although the patient with homocystinuria requires a multidisciplinary follow-up involving a geneticist, nutritionist, pediatrician, or internist [3]. This work aims to present a clinical case of lens subluxation and ophthalmological management, as well as to describe the main ophthalmological characteristics of homocystinuria. Presentation of the case A 35-year-old male patient, apparently healthy parents (not consanguinity) with a personal history of loss of the right eye secondary to a closed ocular trauma at 8 years of age; without further important background. He went to the ophthalmology office due to a sudden decrease in visual acuity in the left eye. Physical examination revealed a marfanoid habit, long fingers predominant in upper extremities, slight brachy-cephaly, scant hair with good implantation, his attitude denotes mental deficiency; no other significant findings (Pic. 1).
In the ophthalmological examination, visual acuity stands out on the count of fingers at 10 cm in the left eye, right eye gutted. In the orbit and periorbital of the left eye with corneal edema ++ / ++++, formed anterior chamber, iridodonesis, and aphakia. Biomicroscopy RE: not assessable, LE: with an IOP of 24 mm Hg. The hydrated lens in the fundus is seen in the left eye (Pic. 2).
Given the clinical presentation of the patient, his mental deficit, and lens dislocation, probable homocystinuria is thought, requesting its determination in blood, which reported a concentration of 285μmol / L (5-16μmol / L), con-firming our diagnosis. Ophthalmological management was implemented with emergency vitrectomy due to increased intraocular pres-sure, migration of the lens to the vitreous chamber, and corneal edema. In the subsequent evaluation of the postop-erative period, the patient evolved favorably, maintaining an IOP of 14 mm Hg although with persistent edema of the corneal endothelium (++ / ++++), so it will be necessary to consider the performance of penetrating keratoplasty. Discussion Homocystinuria is an innate error of metabolism, which can be caused by mutations in at least five different genes: CBS, MMADHC, MTHFR, MTR, and MTRR, in an autosomal recessive form, being the most common cistationin β-synthase deficiency (CBS), this catalyzes the transsulfuration of homocysteine to cystathionine in the presence of pyridoxine, the responsible gene is located in 21 q22.3.2 [4]. The pathophysiological mechanisms responsible for homocystinuria are not exactly known; However, the ele-vation of homocysteine in plasma would be the factor responsible for the main multisystemic clinical manifesta-tions (slow onset and progressive course), this due to the induction of oxidative stress and increased incorporation of homocysteine in different body systems. The clinical picture is characterized by skeletal changes, mental deficit, lens subluxation, and a tendency to thromboembolic phenomena [3]. Regarding ocular alterations, the most common finding is ectopia lentis; it can be accompanied by iridodonesis, diplopia, pupillary blockage, and glaucoma. Subluxation frequently occurs in the nasal and inferior position, for which reason this finding has been considered pathognomonic [5]. The diagnosis is confirmed by plasma homocysteine levels greater than 15 μmol/L. Likewise, there is an eleva-tion of methionine in plasma (homocysteine metabolite), and homocysteine in the urine. The definitive diagnosis is established with the determination of low levels of the enzymatic activity of cystathionine b-synthetase in tissue culture, and with the molecular analysis demonstrating the gene mutation [6]. The systemic treatment of homocystinuria aims to reduce serum homocysteine and methionine levels, thus avoiding cognitive, skeletal, ophthalmological, and thromboembolic complications. The following treatment modal-ities can be used: pyridoxine (50-200 mg 3 times per day), a low-methionine diet supplemented with cysteine, and betaine. Regarding the ophthalmological management of lens subluxation, if it is mild or moderate, the necessary refrac-tion should be prescribed and the patient should be monitored as long as surgical management is not required. The indications for surgery are diplopia, poor visual acuity despite adequate refraction, cataract, corneal edema, subluxation into the anterior chamber or vitreous cavity, glaucoma, uveitis, and retinal detachment. The surgical approach depends on the surgeon's experience, nuclear density, position, and stability of the lens, these include phacoemulsification, intracapsular extraction, extracapsular extraction, lensectomy. Patients with lens subluxation who are treated by surgical procedures are at risk of developing retinal detach-ment, so they require periodic monitoring to detect it. You must always remember the multidisciplinary management that this pathology requires [3].
References 1.Carbajal RL., Barrios FR., Vela AM., Rodríguez HR., Zarco RJ. Homocistinuria: informe de 2 pacientes. Bol Med Hosp In-fant Mex. 2006; 63: 331-326. 2.Gonzalez-Castaño C., et al. Luxación del cristalino: etología y resultados. ARCH SOC ESP OFTALMOL 2006; 81: 478-471. 3.Ortiz-Gonzalez Al., et al. Subluxación de cristalino asociada a homocistinuria: reporte de un caso. Rev. Mex. Oftalmol. 2013; 87 (2): 125-119. 4.Cornejo-Olivas M, et al. Homocistinuria, una enfermedad metabólica de diagnóstico tardío en el Perú. Rev Neuropsiquiatr 2015; 78 (4): 247-240. 5.García GD, Pons CL, Legra NS, Utra PR. Heterogenicidad clinico-genética de la luxación del cristalino. Presentación de tres casos. Rev Cubana Genet Comunit 2012; 6 (3): 58-54. 6.Olivar RJ, et al. Homocistinuria; curso clínico y tratamiento dietético; a propósito de dos casos. Nutr Hosp. 2012; 27 (6): 2138-2133.
The authors did not receive funding for this article. Authors do not have conflict of interest in this article.
|