J.ophthalmol.(Ukraine).2020;6:74-75.
|
http://doi.org/10.31288/oftalmolzh202067475 Received: 23 July 2020; Published on-line: 21 December 2020 Retinal vein occlusion in Crohn's disease Saadouli D, Ben Mansour K, Farae M, Loukil I, El AFrit MA La Rabta Hospital, Tunis E-mail: saadoulid@yahoo.com TO CITE THIS ARTICLE: Saadouli D, Ben Mansour K, Farae M, Loukil I, El A Frit MA. Retinal vein occlusion in Сrohn’s disease. J.ophthalmol.(Ukraine).2020;6:74-5. http://doi.org/10.31288/oftalmolzh202067475 Crohn's disease is an inflammatory bowel disease, which may be associated with a variety of extraintestinal complications, including ocular involvement. However, retinal vascular involvement is noted to be uncommon. We present 2 rare cases of retinal vein occlusion associated with Crohn's disease. Key words: ocular involvement , inflammatory bowel disease , retinal vein occlusion
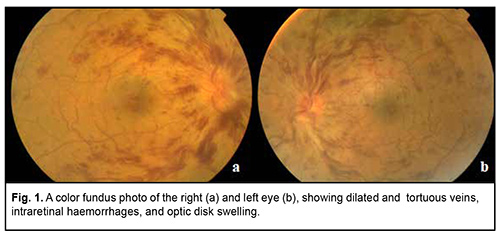
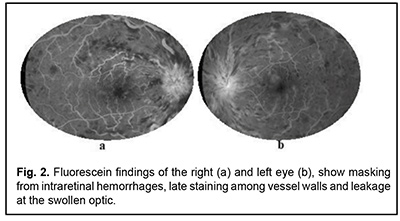
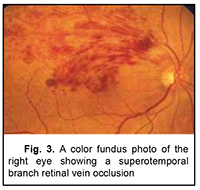
Introduction Crohn’s disease (CD) is an inflammatory bowel disease (IBD) of idiopathic etiolology. Extraintestinal manifestations are frequent. Almost every organ system may be affected [1]. Ocular manifestations during Crohn's disease are polymorphic and occur in about 10% of cases [2]. However, retinal vascular involvement associated with CD is uncommon [3]. We report the cases of two patients presenting a retinal vein occlusion associated with Crohn’s disease. Patient 1 A 27-year-old woman with a 5-year history of Crohn disease. She was in remission for eight months with the oral non-steroidal anti-inflammatory mesalazine. She presented with an acute exacerbation of symptoms and inflammation of the gastrointestinal tract. She was complaining of a concomitant sudden bilateral blurred vision. Visual acuity was 6/10 (Snellen) in her left eye and 4/10 in her right eye. A slit-lamp examination showed no abnormalities. Intraocular pressures were normal in both eyes. The fundus examination revealed disk oedema, retinal flame-shaped haemorrhages, sheathing of the retinal vessels in all four quadrants, and dilated retinal veins (Fig. 1). Fluorescein angiography revealed a prolonged retinal arteriovenous transit time, dilated and tortuous retinal veins, late staining of the vessel walls, and leakage from the disk (Fig. 2). The diagnosis of bilateral oedematous central retinal vein occlusion associated with CD was retained. The diagnosis of this disease was retained after an extensive diagnostic workup. She was treated with oral prednisolone and azathioprine. After 6 months, she improved visual acuity in both eyes. Patient 2 A 21-year-old man was diagnosed as having CD two years prior. At the current presentation, he had a mild disease activity treated by mesalazine. He presented with persistently decreasing vision in his right eye. His visual acuity was of 4/10 in the right eye and 10/10 in the left eye. The slit-lamp examination of both eyes was normal, as well as the fundus examination of the left eye. The fundus examination in the right eye revealed flame-shaped intraretinal haemorrhages located in the supero-temporal retinal quadrant with dilated and tortuous veins (Fig. 3). Etiologic investigations including the coagulation and the immune systems were normal. He was diagnosed with a branch retinal vein occlusion of the right eye associated with CD. Then, he was treated with high-dose intravenous methylprednisolone with a total resolution of his ocular disorder two months after the initial presentation. Discussion Crohn's disease is a multisystem disease. Almost every organ system may be affected [1]. Ocular findings during CD occur in about 10% of cases [2]. A variety of ocular lesions have been described. However, retinal vascular involvement is rare and only few cases of retinal vein occlusion have been reported [3]. Its physiopathology is not well elucidated. Initially, Knox has grouped it under coincidental ocular findings [4]. However, it has been suggested that retinal vein occlusion may depend on the severity of Crohn's disease [5]. In fact, a prothrombotic state may be seen in pro-inflammatory conditions such as IBD [6]. Coagulation abnormalities (increased concentration of coagulation factors) and alteration of vessel walls during IBD lead to a condition of thromboembolism which involves the systemic vasculature as well as retinal veins and /or arterie [7]. In addition, some authors reported that antiphospholipid and antineutrophil cytoplasmic antibodies predispose to vascular occlusive complications in inflammatory bowel diseases, independently of the intestinal activity [6,8]. In the presented cases, due to the young age, the improvement in ophthalmoscopic findings under corticosteroid therapy and in the absence of a clear etiology, the diagnosis of retinal vein occlusion associated with CD was made. There is not yet a well-established therapeutic consensus. According to Chen, 25% of untreated non-ischemic central retinal vein occlusion during IBD, resolved spontaneously at the end of one year [9]. In conclusion, inflammatory bowel disease should be considered among the causes of retinal vein occlusion especially in young patients and in absence of clear etiology. Early and regular ophthalmic examination is required in patients with IBD to establish an early diagnosis and to start an adequate treatment.
Bibliography 1.Mintz R, Feller ER, Bahr RL, Shah SA. Ocular manifestations of inflammatory bowel disease: Inflammatory Bowel Diseases. mars 2004;10(2):135 9. 2.Felekis T, Katsanos K, Kitsanou M, Trakos N, Theopistos V, Christodoulou D, et al. Spectrum and frequency of ophthalmologic manifestations in patients with inflammatory bowel disease: A prospective single-center study: Inflammatory Bowel Diseases. janv 2009;15(1):29 34. 3.Abdul-Rahman AM, Raj R. Bilateral retinal branch vascular occlusion—a first presentation of crohn disease: Retinal Cases & Brief Reports. 2010;4(2):102 4. 4.Knox DL, Schachat AP, Mustonen E. Primary, secondary and coincidental ocular complications of Crohn’s disease. Ophthalmology 1984; 91 (2): 163-73. 5.Igarashi H, Yanagawa C, Igarashi S. Crohn's disease and central retinal vein occlusion.Indian J Ophthalmol 1996;44:97-99 6.Lapsia S, Meyer R, Abazari A, Usmani K, Gathungu G. Bilateral central retinal vein occlusion in a patient with ulcerative colitis and antiphospholipid antibody syndrome: Journal of Pediatric Gastroenterology and Nutrition. mars 2016;62(3):e25 6. 7.Zezos P. Inflammatory bowel disease and thromboembolism. WJG. 2014;20(38):13863. 8.Greenfield SM, Teare JP, Whitehead MW, Thompson RPH. Amaurosis fugax, crohn’s disease and the anticardiolipin antibody. Lupus. févr 1993;2(1_suppl):271 3. 9.Chen JC, Klein ML, Watzke RC, Handelman IL, Robertson JE. Natural course of perfused central retinal vein occlusion. Can J Ophthalmol. févr 1995;30(1):21 4.
Received 23.07.20
No conflict of interest was declared by the authors.
|