J.ophthalmol.(Ukraine).2020;5:90-96.
|
http://doi.org/10.31288/oftalmolzh202059096 Received: 15 June 2020; Published on-line: 27 October 2020 Vladimir E. Shevalev, the disciple Academician V.P. Filatov loved N.F. Bobrova1, V.V. Shevaleva2 1 Filatov Institute of Eye Diseases and Tissue Therapy, NAMS of Ukraine; Odessa (Ukraine) 2 Research and Practice Center for Preventive and Clinical Medicine of State Administration of Affairs; Kyiv (Ukraine) TO CITE THIS ARTICLE:Bobrova NF, Shevaleva VV. Vladimir E. Shevalev, the disciple Academician V. P. Filatov loved. J.ophthalmol.(Ukraine).2020;5:90-6. http://doi.org/10.31288/oftalmolzh202059096 Vladimir Evgenievich Shevalev (Fig. 1) was the third generation of his family to be born in Odessa. His father, Evgenii Aleksandrovich Shevalev (Fig. 2), Professor and Chair of Psychiatry at Odessa Medical Institute, was acting medical superintendent of the city mental hospital and performed an act of civil courage during the Nazi occupation of the city during the Second World War. Evgenii Shevalev managed to forge the medical records of Jewish patients with the help of his younger son Andrei and hospital personnel, and, by the year of 1942, there was no Jew among officially registered patients of the hospital, and the latter continued admitting “new” patients. The exact number of persons saved by the Shevalevs and hospital personnel is still unknown. Many years later Israel’s Yad Vashem Holocaust Martyrs’ and Heroes' Remembrance Authority awarded Evgenii Shevalev and his younger son Andrei the title of Righteous among the Nations.
Vladimir’s mother, Evgeniia Nikodimovna, a graduate of the Bestuzhev’s courses, was among the first female students to enroll at and graduate from the Medical School of Lausanne University. She worked with her husband in St Petersburg at the Psychoneurologic Institute. After they moved to Odessa, she worked at the psychology department of the university, and studied psychology of children teams and children’s creativity. In addition, she was actively engaged in social activities, combating homelessness, establishing labor communities, and was elected to the city council in Odessa. The Shevalevs family was industrious and disciplined. Children were taught to respect labor and cooperativeness. Vladimir applied for enrollment to the maritime academy because, like many other boys in Odessa, he had been dreaming of becoming a seaman since he was a kid, but his mild myopia was the reason why he failed to pass medical examination and was rejected. Thereafter he accepted his father’s advice to enter the medical institute with a notion of becoming a ship’s doctor. After graduating from the medical institute in 1931 and completing maritime medicine courses, Vladimir started working as a ship doctor on long-voyage (Fig. 3) and coastal vessels. He began gaining experience in numerous medical fields because as a ship’s doctor he had to provide care for various traumas, diseases, infections in the setting where there was nobody to ask for advice.
He made several voyages across the Atlantic as a ship’s doctor, and visited US cities like New York, Philadelphia and Jacksonville. Particularly, he visited American medical clinics and physiology laboratories, where from he brought the literature that was current at that time to Academician Ivan Petrovich Pavlov, the founding father of Soviet physiology, who was well known and respected not only in Europe, but the New World as well. Back then, Vladimir displayed his interest in studies on human body response under unusual conditions. This resulted in his first reports, particularly, at the Black Sea conference of physicians in 1933 (Cephalography as a technique for diagnosing predisposition to sea sickness; in collaboration with R.O. Faitelberg) and 1935 (On the effect of cerebral anemia on conditioned-reflex activities; in collaboration with M.V. Los). A chance encounter with Acad. V.P. Filatov on board the motor vessel Adzharia changed Vladimir Shevalev’s subsequent life. Vladimir Petrovich Filatov could make young physicians devoted to his numerous research projects on the potential for restoring vision in blind individuals. The point of those summer evening conversations was discussing the potential for the development of corneal transplantation procedures. The interlocutors became interested in and liked each other. At the end of this encounter, V.P. Filatov invited the young ship’s doctor to work at the Department of Ophthalmology, Odessa Medical Institute. Vladimir became a registrar of the department, and soon was up to his ears in clinical and therapeutic research activities (Fig. 4). In the clinic he learned new surgical techniques for cataract, glaucoma, and, certainly, corneal transplantation. Acad. V.P. Filatov’s achievements in corneal transplantation attracted numerous blind people with corneal leucoma from all over the USSR and abroad to Odessa, but the resources available at the clinic were found to be limited for adequate response. The need to build and establish the Institute of Experimental Ophthalmology (subsequently, the Filatov Odessa Research Institute) has become acute, and V.E. Shevalev actively participated in the idea by monitoring the construction process and making corrections in the project documents.
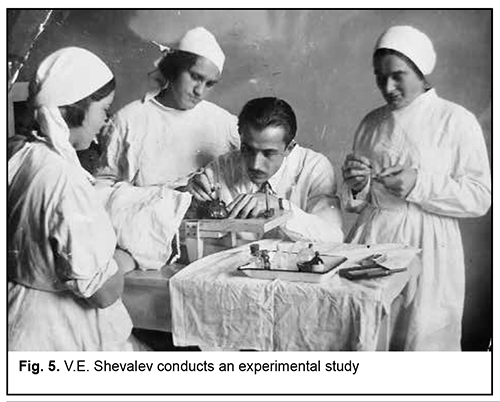
In 1936, the research institute was established in Odessa on the initiative of V.P. Filatov, and V.E. Shevalev became one of its first employees. He was entrusted by V.P. Filatov to head the laboratories of the institute. His research interest was still physiology, particularly, the effect of muscle fatigue on regulation of intraocular pressure (IOP). Acad. V.P. Filatov with his disciples I.G. Iershkovich and O.G. Fishner noted decreased IOP in runners after serious sport competitions and/or training sessions. Studies by V.E. Shevalev (Fig. 5) demonstrated that muscle activity caused a decreased IOP in rabbits and dogs, confirming the Filatov’s hypothesis on the effect of muscle activity on the IOP. In addition, studies in patients with glaucoma confirmed the results of animal studies, leading to the conclusion that these patients require not rest but controlled muscle activity. In 1938, V.E. Shevalev completed his Cand Sc (Med) thesis Experimental Studies on the Effect of Muscle Activity and Fatigue on the IOP under the mentorship of V.P. Filatov, and successfully defended it.
While working at the clinic, he struck an acquaintance with Valentina Pavlovna Getman who had been with the institution since 1923, working her way up from a messenger to ophthalmologist (Fig. 6). He fall in love, they married, and she became a faithful wife and mother for their children.
Trachoma, a chronic ocular infection affecting the conjunctiva and cornea, was a disaster in the nineteen thirties, causing blindness in children and adults. It is an anthroponotic disease spreading epidemically, and is caused by Chlamydia trachomatis, the organism that was discovered in 1907 and propagates in conjunctival and corneal epithelial cells. The condition was well known to ancient writers, and was widely spread in tropical and subtropical regions. It was given Greek name trachoma, from the Greek traxus, “rough”, and this refers to the appearance of the upper tarsal conjunctiva of patients with trachoma. The disease is related to poverty, overcrowding and poor hygiene. Chlamydia trachomatis can be spread by either direct contact with an infected person's eyes or nose or indirect contact, such as via contact with clothing or flies that have come into contact with an infected person's eyes or nose. The disease came to prominence in Europe during the Napoleonic Wars when tens of thousands of British and French troops returned with trachoma after fighting in Egypt, and the so-called Egyptian inflammation of the eye spread first in the army and then among civil population. In the early nineteen century, tens of thousands of persons became blind because of trachoma. V.E. Shevalev and V.P. Getman were doctor members of the so-called mobile team headed by Prof. K.P. Tsykulenko which was sent from the Department of Eye Diseases to Turkmenia to combat the disease. V.P. Filatov developed follicle equalization method that changed the treatment paradigm for trachoma at that time. Doctor members of the mobile team had to work hard from early morning until late in the day. Donkeys were the main means of transportation. They were loaded with unsophisticated medical equipment and the necessaries of life, and in this way, the team was coming from one village to another to perform treatment, educational and organizational activities. The workload of team members was high since there were numerous patients with trachoma and other ocular disorders. Such mobile team tours were conducted in 1937 and 1939. In these tours, mobile team members were conducting medicamentous and surgical treatment through removal of trachomatous follicles, involving local ophthalmologists and other medical specialists in these procedures, and promoting hygiene practices. This helped get things moving. The trachomatous institute (currently, the Turkmen Institute of Eye Disease) was established, and became the major ophthalmology center in the Central Asia. The Experimental Research Institute of Eye Disease that had been established in Odessa continued to evolve in multiple areas, but the war began on June 22, 1941. In July, 1941, V.P Filatov and a portion of his disciples were evacuated to the Caucasus and then to Tashkent, were the activities of the institute were partly restored. In addition, a hospital for wounded with eye injuries was established at the building of the institute in Odessa, and was headed by Assistant Professor V.E. Shevalev within the period of the defense of Odessa (Fig. 7). Vladimir wrote in his Hard Days and Nights of Odessa memoirs that, after daytime bombing, the city was becoming revived at night, and the new wounded were being delivered to the new building of the institute, their number often approaching five hundred a night. The ophthalmic surgeons had to provide care not only for eye wounds, but also for chest, abdomen and extremity wounds, etc. Small-size eye surgery instruments were not suited for large surgery. In addition, ophthalmologists had to revive their knowledge of military surgery. Besides the hospital chief medical officer, the medical hospital team working shoulder-to-shoulder included his father E.A. Shevalev, professor of psychoneurology, and brother A.E. Shevalev, a biology student; Professor I.M. Sribner and Professor M.K. Lisenko; military surgeons Weisberg and Chernigovskii; L.M. Lipkin, a ship’s doctor; M.T. Shendrik, a head surgery nurse; and young specialists O. Kovalchuk, E. Morgunova and E. Slavinskaia. All team members kept working hard, sparing neither time nor efforts. A blood donor center was established at the hospital on the order of V.E. Shevalev. Hospital doctors, nurses and attendants became blood donors, and V.E. Shevalev was the first to donate his blood at the donor center. Thousands of wounded persons were the patients of the hospital within the period of the defense of Odessa. On the night of November 16, 1941, a portion of the hospital staff (including V.E. Shevalev) was evacuated from Odessa to the besieged town of Sevastopol. Surgeon V.E. Shevalev was performing surgery for wounded defenders of Sevastopol at the hospital located at the Inkerman adits…
Then he was taken prisoner and sent to a concentration camp by the Nazis. After the Soviet troops liberated Sevastopol, he was sent to a Soviet concentration camp and prison. An interesting paper issued by the NKVD for V.E. Shevalev was preserved from that time, and was to certify that Dr. V.E. Shevalev, a military doctor of the second rank, had passed through a check by the SMERSH counterespionage service without arousing suspicion. He was rehabilitated and given back his combat awards (the Order of Red Combat Banner, Medal for Combat Service, Medal for the Defence of Odessa, and Medal for the Defence of Sevastopol), but was left to work at the medical sanitary unit of the NKVD. Dr. V.E. Shevalev’s demobilization and release for coming back to his work at the Filatov institute was obtained on intervention from the Acad. V.P. Filatov. While heading up the Trachomatous Department of the institute, Vladimir Evgenievich paid attention to cicatricial xerosis, a final phase of trachoma, pemphigus and some other chronic inflammations of the conjunctiva and sequelae of burns to the eye. He had seen a lot of such patients as a member of mobile teams combating trachoma in Turkmenia. At that time, doctors could not help patients with cicatricial xerosis, with available methods and surgical techniques providing only temporary improvements. Acad. V.P. Filatov proposed to try using the saliva from the patorid gland instead of the tears secreted by the lacrimal gland in these patients. The successful transplantation of the parotid duct into the conjunctival sac was preceded by a lot of work: anatomical and physiological features of both glands were studied, physical and chemical composition and function of tears compared with those of the saliva, and topography, innervation and blood supply of the parotid duct studied, etc. After successful dog studies, investigators conducted studies on cadavers. In 1950, they started performing surgeries for cicatricial xerosis in humans. In the first patient, one eye was blind due to cicatricial xerosis, whereas the other eye was dead. The cornea started becoming clearer and the patient obtained some vision in her eye as a result of continuous eye moistening with the saliva. The developed technique was atraumatic and physiological. In addition, in order to facilitate the procedure, investigators developed special scissors with a hole in the branch for one-step transfer of the separated duct through the newly developed hypodermic canal to the inferior conjunctival fornix (Fig. 8).
However, they succeeded in avoiding late scarring of the duct only approximately in half of the 70 patients that underwent the procedure. Investigators had to develop a new technology for restoring duct patency. Moreover, the amount of secreted saliva had to be regulated as some patients were secreting too much saliva. In order to solve the problem, it was proposed to expose the parotid gland area to X-rays. Methods were being developed to conduct optical procedures (iridectomy and corneal transplantation) on the eye moisturized with saliva. This extensive material was formalized and organized into a doctoral dissertation, but Vladimir Evgenievich did not have sufficient time to defend it while Acad. Filatov was alive, and various legal issues arose after the latter’s death. Nevertheless, the dissertation was successfully defended at the Kuibyshev Research Institute of Eye Diseases headed by Professor Tikhon Ivanovich Eroshevskii. Eroshevskii was a person capable of scientific prevision, and it was he who later supported a future academician S.N. Fedorov with a “crazy idea” of artificial lens implantation in cataract surgery. This surgical technique has been considered a routine procedure since the late twentieth century. In 1959, V.E. Shevalev published a monograph entitled “Cicatricial xerosis of the eye” with a run of 2,750 copies in Russian. The Shevalev’s technique of transplantation of the parotid duct into the conjunctival sac for the treatment of cicatricial xerosis was subsequently utilized by numerous ophthalmological institutions over the USSR and in Poland, Bulgaria, Romania, China, USA, the Netherlands, India, etc. In 1962, the monograph was translated into English and published in New York, an extremely rare event at that time.
Soon after completing the research on the treatment of cicatricial xerosis, Shevalev became busy with studies on the surgical treatment of retinal detachment. The issue was really important as retinal detachment was accompanied by irreversible loss of vision and sometimes even loss of the eye. In 1931, V.P. Filatov and M.I. Averbakh were the first in the USSR to treat retinal detachment surgically by Gonin’s method. Briefly, the procedure included excising the sclera at full thickness at the site of retinal hole, followed by draining out the subretinal fluid, and cauterizing the retina through the sclera. Gonin's technique involved the closure of retinal holes by the formation of adhesions between the choroid and retina. There appeared a real opportunity to repair retinal detachments. During Gonin’s era, the success rate was reported to be as high as 39-54 %. However, clinical application of the technique was limited since it could be used only in fresh and mobile retinal detachments with a single small hole, and did not work in multiple holes or old (rigid) detachments. The majority of procedures for the next 20 years were variants of Gonin’s operation with modifications in the method of treatment of breaks and the method of drainage. There were techniques aimed at reducing the volume of the globe by lamellar or penetrating scleral resection; indentation of the sclera and invagination with sewed-on buckles were aimed at bringing the retina and choroid close together. Saline or air was injected into the vitreous to hold it in place. Scleral diathermy and other methods were being modified. Meyer-Schwickerath, in 1949, was the first to publish the technique of photocoagulation. He designed a photocoagulator that used a narrow light beam passing through the transparent ocular media to obtain fusion of the retina and choroid under visual control of the physician, which was especially important. V.E. Shevalev can be considered as a father of national retinology, since he began solving the problem of surgical treatment of retinal detachment, as they say, from the very beginning. By that time, he headed the 4th department of the institute (the retinal detachment department) which was staffed mostly with young ophthalmologists (Yunona Dmitrievna Babanina, Svetlana Fedorovna Vasilieva, Nina Semenovna Kalfa, Leonid Andreevich Linnik, and Sergei Vladimirovich Filatov). They were learning to perform ophthalmoscopy and identify retinal holes and tears. In addition, they were developing methodologies for localization of holes and transfer of projection of the hole to the sclera surface and determining indications and contraindications for surgery. What was most important, proprietary techniques were developed to improve the retinal reattachment rate. Of particular note are the methodologies developed for scleral indentation using catgut invagination, modified lamellar sleral resection, hot scleral indentation, dosed scleral diathermocoagulation, air or silicon injection into the vitreous, etc. Back then ophthalmologists were in search of opportunities for vitreous tamponade and being developing a methodology for vitreous transplantation from cadavers for retinal reattachment. In 1965, V.E. Shevalev and Y.D. Babanina published a monograph entitled Surgical Treatment of Retinal Detachment with a run of 5,000 copies in Russian, which contained descriptions with detailed schemes, intraoperative and postoperative complications, and treatment outcomes for relevant surgical techniques. In addition, cases were reported and discussed, and patient behavior requirements, features of postoperative employment of patients and retinal detachment prevention addressed. The monograph has become a reference book for the ophthalmologists dealing with retinal detachment, high myopia, peripheral retinal degeneration, etc. All the disciples of V.E. Shevalev defended Cand Sc (Med) theses or Dr Sc (Med) dissertations. Vladimir Evgenievich was the heart and leader of the institute and used to organize weekend trips for the staff. Early in the morning they were leaving the city on a lorry (one could only dream of a bus at that time) that was going to Tiligul estuary (for fishing) or Zatoka. However, to arrive early to the market in Vilkovo, they were leaving Odessa in the evening and had to sleep at night in the field in a haystack. Shevalev was the heart and leader of any company or discussion. He knew the outskirts of Odessa quite well, and, when requested by Acad. V.P. Filatov, used to find “nice places”, and bring the academician to these locations for plein air sketching. To this date, one can see numerous paintings created by V.P. Filatov on the basis of these sketches on the walls of his memorial home on Frantsuzskii boulevard in Odessa. Shevalev understood painting well, was painting a little bit and even writing poetry, and fond of classic music. His love for art helped him finding his way to get into one’s soul and getting a wonderful bed-side manner. In the last years of his life, V.P. Filatov was often sending V.E. Shevalev on business trips to consult famous figures. Thus, Shevalev consulted Archbishop Luke (Professor V.F. Voino-Yasenetsky) in Simferopol; Ioann, Metropolitan of Kyiv and All Rus, in Kyiv; Archbishop Juvenal in Vilnius; Metropolitan Nestor in Kirovograd, etc. Although Vladimir Evgenievich was not a committed Christian, he, with his family, had a tradition of visiting the Easter service held at the Filatov’s church on Frantsuzskii Boulevard. Having stand throughout the entire service, they were visiting V.V. Skorodinskaia, the Filatov’s wife and godmother of Vera (V.E. Shevalev’s daughter), at the Filatov’s house. In his time, Vladimir Evgenievich was best man at the wedding ceremony of Acad. V.P. Filatov and V.V. Skorodinskaia which was held at the ancient church in Georgia in between the sessions of an ophthalmology congress. After V.P. Filatov fell to the floor at the corridor of the institute, Vladimir Evgenievich lifted him up in his arms, carried him to his home nearby, and was staying each night by his teacher’s bedside until his death. The words V.P. Filatov told him in 1953 were worth remembering: “Vladimir Evgenievich, your encounters with patients will be remembered for long or even forever. The special ease with which you can pour consolation and hope into each patient’s heart will guide us in our everyday life. Leaving an image of a light, noble and cordial doctor in the patient’s heart is the greatest award possible for a doctor. You do have plenty of these awards”. Vladimir Evgenievich loved Odessa, the city he was born in and his numerous relative lived in, he loved the institute and institute staff, his teacher and his disciples, and the Black Sea. In those years, the institute had boat moorings at the nearby sea coast, and Vladimir Evgenievich was taking sea trips with his family on a red-scarlet boat named Votalif (i.e., Filatov when read from the right to the left) to the area of Lustdorf (now Chernomorka), Ochakov, and the island of Berezan. They were fishing bullheads; mackerel was easy to catch with multi-hook rigs. The eldest son of Vladimir Evgenievich liked the sea so much that after graduating from his school he enrolled in the maritime academy. The climate in the institute has begun to change after Acad. V.P. Filatov had passed away, and Shevalev understood that he had to leave the institute. The decision was made due to not only subjective factors. The objective factor was that he was a free and creative person, the person that (1) sought to go beyond whatever was given in the immediate environment to create something new, (2) got accustomed to make his decisions himself, and (3) felt himself uncomfortable when being limited by administrative framework. He had numerous propositions for employment, but decided to leave for Kyiv and accept the proposition of P.L. Shupik, then-Minister of Health of Ukraine, to head the Department of Ophthalmology at the Institute of Continuing Education for Medical Doctors. After he became the Chief Ophthalmologist of Ukraine, he established the Department of Ophthalmology at the newly constructed buildings of the Medical Town, which subsequently was transformed into the now well known Eye Microsurgery Center. In addition, he continued his surgical activities, established a new ophthalmology school dealing with various areas including retinal detachment, and invited a young doctor from Dagestan, Nikolai Markovich Sergiienko, to work at the Institute of Post-graduate Education. But that is another story. So what kind of affinity did Professor V.E. Shevalev have with Acad. V.P. Filatov, and why the former was the disciple the latter loved? The answer is as simple as complex: it was the affinity of souls, they were soul mates. Both of them were descendants of distressed nobility, polymathic and industrious persons persevering in attaining their goals and inflamed with an idea of making blind people see again. They were talented surgeons with excellent skills and a pioneering spirit, splendid lecturers, story tellers, and teachers, kind, charming, full of compassion and benevolence, loving all people and things. They loved nature, the sea, painting and art in general, and found art both as a way to find some rest and as an inspiration for further research. And was it by chance that they lived in the same house on Gogol Street in Odessa before the war?
|